How to avoid autopsy and long ‘down-time’
(ischemia) better than ~85% of the time!

By Mike Darwin
Ischemia: The Problem of “Long Down Time”
Almost every cryonicist I’ve ever spoken with envisions his cryopreservation will occur under ideal circumstances. He will be diagnosed with some vague and ill defined terminal illness, bravely decide to end futile treatment and then enter hospice with a team of skilled and caring cryonics personnel at his bedside. He will nap, read, watch TV, and then, near the end, nod off surrounded by loved ones as the cryonics personnel hover nearby. This may not be the most attractive picture in any absolute sense, but it is certainly as reassuring a one as it is possible to find in contemporary cryonics. And while many, or even most cryonicists may find this scenario credible, much of the rest world doesn’t.
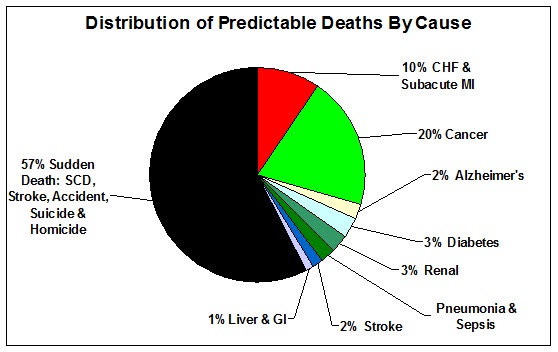 Figure 10: Approximate U.S. distribution of predictable deaths by cause based on 2004 data. Note that ~57% of all deaths occur sufficiently suddenly, or under circumstances such as accidents, which preclude standby or other cryonics stabilization measures. Chart derived from data: [National Vital Statistics Report, Volume 53, Number 5 (October 2004)]. This data may be compared to the data in Figure 10 to see how closely the US national incidence of sudden and unpredictable death map that of Alcor’s experience (Figure 11).
Figure 10: Approximate U.S. distribution of predictable deaths by cause based on 2004 data. Note that ~57% of all deaths occur sufficiently suddenly, or under circumstances such as accidents, which preclude standby or other cryonics stabilization measures. Chart derived from data: [National Vital Statistics Report, Volume 53, Number 5 (October 2004)]. This data may be compared to the data in Figure 10 to see how closely the US national incidence of sudden and unpredictable death map that of Alcor’s experience (Figure 11).
One likely reason for the scarcity of biomedical people involved in cryonics is that their actual, day-to-day experience is at sharp odds with the scenario I’ve just laid out above. In countless hours of both focused and casual conversations with such individuals, what emerges is a sense of incredulity about the reversibility of the damage these professional and technical people witness as a part of their duties caring for the very old, and the critically ill dying; not to mention that large fraction of people who die suddenly and without warning, end up as DOAs in the emergency department or coroner’s cases. Regardless of whether their opinions prove the valid ones, we are clearly failing to communicate to them and to the community at large, an experience of cryonics which is not so biomedically adverse.
To do that, it is first necessary to move beyond anyone’s scenarios or suppositions and evaluate the reality of what is actually happening to the patients we cryopreserve. That turns out to be a hard thing to determine with any degree of precision, because none of the cryonics organizations maintain any kind of statistical database on their members’ cryopreservations. How many cryopatients have dementia? How many were autopsied? What is the mean ischemic time from cardiac arrest to the start of cardiopulmonary support (CPS)? How many patients have ischemic times of 2-5 minutes, 5-10 minutes, 15-30 minutes, 12 hours, 14 hours, 5 days? What is the mean age at cryopreservation? [Absence of data on this last question I find particularly amusing in a group of people supposedly preoccupied with longevity and "life extension": how long are they living, on average?] There is currently no way to tell.
There is not even any way to determine the age, gender, or any of dozens of other potentially critically important demographic details that are, or could be vital in assuring quality cryopreservations, reducing ischemic times, or reducing known iatrogenenic events. A concern of mine for onto three decades now is that we have no way to spot adverse epidemiological events that might be associated with our unique dietary supplement or other lifestyle practices. Perhaps most incredibly, there are no written criteria, however arbitrary, to assign any degree of quality, or lack thereof, to the cryopreservation a given patient has received (let alone that a given Cryonics Organization (CO) provides, on average). This had lead to what has become known as “the last one is always the best one” to date rating system, wherein each case that is not either an existential or an iatrogenic disaster, is pronounced by the staff who carried it out as, “the best case we’ve done so far!”
We cryonicists may be in some kind of willful, data free fog about what our situation is, however, it’s a safe bet to assume that most of the rest of the world, based on their own professional and personal experiences, are not so ignorant. The first step towards a solution is to understand the scope and severity of the problem by getting reliable numbers. While that is not easy to do, the Alcor Life Extension Foundation does maintain a crude, if incomplete accounting of all the patients they have placed into cryopreservation: http://www.alcor.org/cases.html. A cursory analysis of this yields the following breakdown. Even basic data such as cause and mode of death are missing from ~20 of the cases listed there – these have necessarily been excluded from the analysis below.
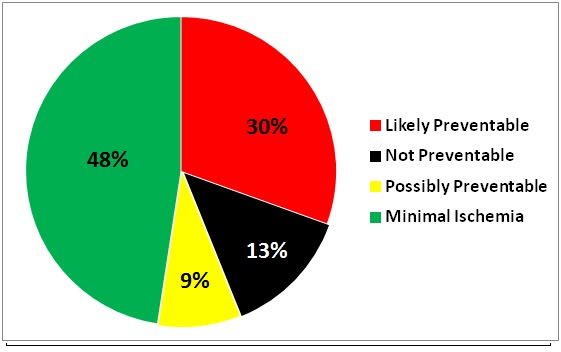 Figure 11: A major hurdle to evaluating quality in cryonics operations is the lack of any outcomes (e.g., reanimation followed by evaluation) or of any surrogate markers or scoring systems to serve as evaluation tools to determine not only the quality of cryopreservation care being given, but also the objective neurocognitive status of the patients when they enter cryopreservation. For the purposes of this analysis very crude criteria were used to assess the quality of the patient as a finished product at the end of cryopreservation. These were normothermic ischemic time between cardiac arrest and the start of CPS, catastrophic peri-arrest brain injury such as an intracranial bleed followed by prolonged cerebral no-flow before pronouncement of medico-legal death, very long warm ischemic times (> or = to 12 hours) and autopsy.
Figure 11: A major hurdle to evaluating quality in cryonics operations is the lack of any outcomes (e.g., reanimation followed by evaluation) or of any surrogate markers or scoring systems to serve as evaluation tools to determine not only the quality of cryopreservation care being given, but also the objective neurocognitive status of the patients when they enter cryopreservation. For the purposes of this analysis very crude criteria were used to assess the quality of the patient as a finished product at the end of cryopreservation. These were normothermic ischemic time between cardiac arrest and the start of CPS, catastrophic peri-arrest brain injury such as an intracranial bleed followed by prolonged cerebral no-flow before pronouncement of medico-legal death, very long warm ischemic times (> or = to 12 hours) and autopsy.
Using the criterion of “minimal ischemia” (≤15 minutes)[1], 48% of Alcor’s patients are cryopreserved under these conditions (Figure 10). Thirty-nine percent of their patients suffer long ischemic periods of 6-12 hours or more (mostly as a result of SCA and UDA); and 13% suffer very long periods of ischemia (> or = to 24 hours) which are not currently preventable, or which conclude in autopsy prior to cryopreservation. Put more cogently, you have less than a 50% chance of being cryopreserved (with Alcor) under conditions of minimal ischemia. While this number is discouraging, it is spectacular when compared to the Cryonics Institute, where it is somewhere in the low single digits.
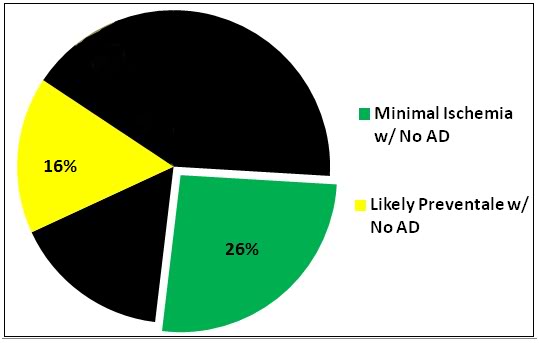
Figure 12: The graph above is the same as in Figure 11, with the difference being that the losses have been expanded to include those that would be expected if the population wide incidence of end-stage, GDS-7 dementias were imposed on all the groups. The result is that percentage of patients who might reasonably be expected to have both minimal ischemia and no pre-cryopreservation GDS-7 dementias drops to just 26%.
But once again, these numbers are misleading if the criterion is cryopreservation under minimal ischemia conditions, because they do not take into account the number of patients who enter cryopreservation with dementia, or severe brain injury due to stroke, other neurovascular disease, or massive head trauma. If only dementia, at the current incidence for the general population is factored into the analysis, then the picture becomes considerably more bleak, as can be seen in Figure 10, with only 26% of Alcor cryonics patients being preserved with relatively intact brains under reasonably good conditions.[2]
Impact of the BDDs on the Likely Survival of Personhood
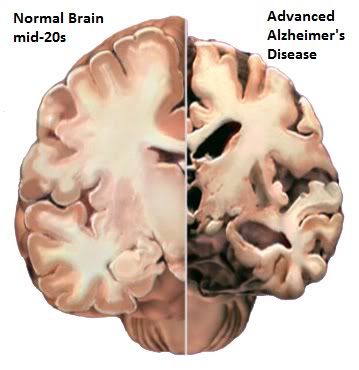
Figure 13: The effect of advanced Alzheimer’s Disease on the macroscopic appearance of the brain is evident when coronally sectioned brains from an AD (R) patient and a healthy person in their mid-20s (L) are compared side by side.
Deaths from AD are typically deaths from end-stage AD, which usually implies severe global destruction of both cerebral hemispheres (Figures 13 & 14) on both a macro and microscopic level. Death due to AD is a prolonged process (~8 years from diagnosis to death), and the neurological deterioration that occurs as the disease progresses is often scored using the global deterioration scale (GDS) of primary degenerative dementias, which ranges from 1 (least) to 7 (worst) in severity. GDS scores in excess of 5 are associated with major loss of macro- and micro-scale brain structure and will be assumed here to represent serious compromises to, or the destruction of personhood.
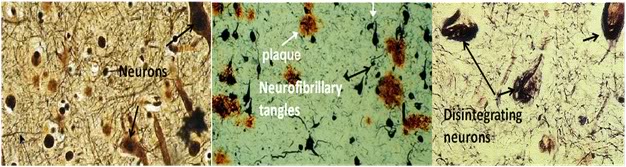
Figure 14: The histological appearance of the brain in AD is shown in panels b and c above. In many areas of the brain there is virtually complete loss of the neuropil; the synaptic weave that interconnects neurons which can be seen in its normal state in c, the panel at the far left. The majority of the neurons and many of their supporting glial cells have died and been scavenged by macrophages and histiocyytes. There are abundant deposits of proteinaceous plaque containing the neurotoxin protein beta amyloid neurofibrillary tangles which are the remnants of neuronal long processes such as axons and dendrites. The extent and uniformity of the changes seen above varies from patient to patient during the course of the disease, but becomes increasingly uniform throughout both hemispheres of the cortex the longer the patient survives with a GDS score of 7 (end stage dementia).
A Deanimation Warning Device?
Figure 15: The medical imager as a deanimation prediction device?
In his 1939 science fiction story Life-Line,” Robert Heinlein envisions a device that can predict, with considerable precision, when a person is going to die. While none of us cryonicists wants to die, most of us could certainly profit from knowing when we are going to deanimate. Better still would be also finding out how to postpone our cold dip in liquid nitrogen for a while, if it was possible to do so.
Many cryonicists will be familiar with this graph of Ray Kurzweil’s showing the impending arrival of the singularity (Figure 16).
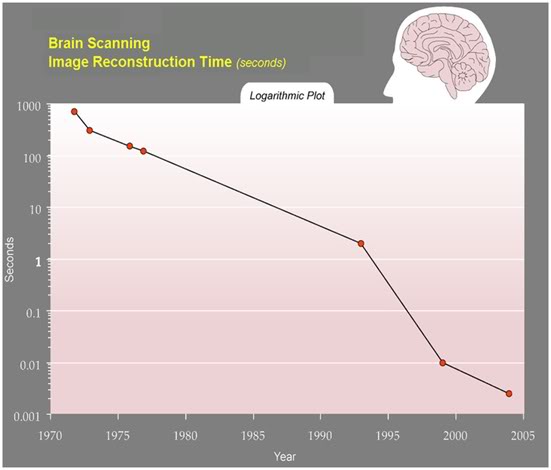
Figure 16: Ray Kurzweil’s graph showing the exponential increase in neuro-image reconstruction which has occurred largely as a function of the exponential growth in computing capacity since 1970.
Well, if you are a cryonicist, I’m here to tell you that insofar as non/minimally-invasive medical imaging is concerned, the singularity is here.
From the earliest days of medicine physicians have desired one thing almost above all others and that is to possess the power to peer into their patients bodies and observe the goings on there. Since the discovery of x-rays by Wilhelm Conrad Röntgen in 1895 (Crane, 1964) there has been steady progress towards the satisfaction of that desire. The development of contrast media, endoscopy, computerized axial tomography (CAT or CT) scanning and magnetic resonance imaging (MRI) scanning have allowed increasingly exact and impressive images of the interior of the living body to be made.
However, a number of serious limitations have, and to a great extent still do prevent the full realization of the physician’s idealized desire to see inside his patients at will. Those barriers are field, dimensionality and point of view, as well as resolution, color, contrast and the dollar cost of the imaging.
In the case of CT and MRI those barriers have been breached to such a degree that it is now possible for cryonicists to be able to determine with a very high degree of accuracy and precision both of what and when they are going to experience medico-legal death. A corollary of this is that in many cases it will be possible for them to avoid what would have otherwise been an unavoidable very long period of ischemia and quite likely a medico-legal autopsy as well.
End of Part 2
[1] This criterion is being very generous because it assumes that all interventions that begin within ~15 min of cardiac arrest are effective at preventing further ischemic injury. This is not the case for most cryonics patients where external cardiopulmonary support is not effective at restoring adequate perfusion and gas exchange, core cooling may be delayed by several hours, and cold ischemic times may be in the range of 12 to 24 hours.
[2] Again, using the very generous criteria of assuming that all CPS is effective CPS and that no iatrogenic events compromised the quality of the cryopreservations.
